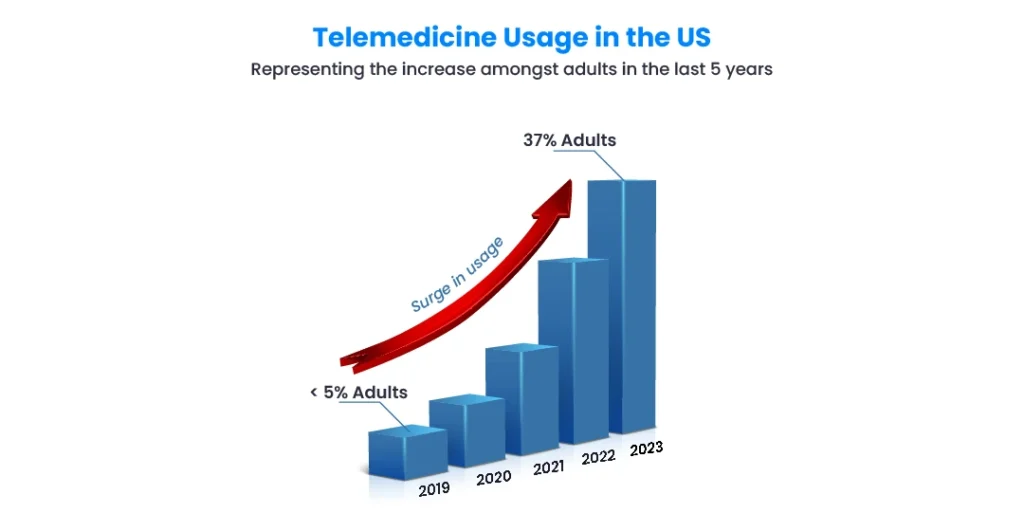
The Rise of Telemedicine in the USA: Transforming Healthcare Delivery
Telemedicine, which refers to the use of telecommunications technology to provide remote healthcare services, has been around for decades, but it was the COVID-19 pandemic that truly accelerated its growth and integration into mainstream healthcare in the United States. Prior to the pandemic, telemedicine was already making strides, particularly in rural areas and for certain types of consultations. However, as hospitals and clinics scrambled to adapt to the crisis, telemedicine became a crucial tool in maintaining access to healthcare while minimizing the spread of COVID-19.
As we move into 2026, telemedicine is no longer a temporary solution but has become a permanent fixture in the healthcare landscape. This article will explore the rise of telemedicine in the USA, its impact on healthcare delivery, challenges, regulatory changes, and its future potential.
The Growth of Telemedicine in the USA: A Historical Perspective
Telemedicine is not a new concept. The idea of providing healthcare remotely dates back to the 1950s when early experiments were conducted in space programs and with radio technology. These initial efforts aimed to support astronauts and remote workers, but the foundational technologies for telemedicine—such as phone consultations and remote diagnostics—were born in these early years.
In the 1990s, as the internet became widely accessible, telemedicine began to find its way into more practical applications. Early telehealth services focused on specific conditions like mental health therapy, dermatology consultations, and follow-up care for chronic illnesses. However, telemedicine was still in its infancy, limited by technology barriers, limited reimbursement by insurance companies, and regulations that varied by state.
Pre-COVID Landscape
Before the COVID-19 pandemic, telemedicine adoption was slow but growing. The rise of high-speed internet, mobile technologies, and smartphones created new opportunities for virtual healthcare. Telemedicine services were commonly used in rural areas, where access to specialists and healthcare facilities was limited. Many rural residents relied on telemedicine for consultations with doctors, as traveling long distances to access healthcare was not always feasible.
Insurance companies had started covering telemedicine visits in select situations, especially for mental health services. The expansion of telemedicine was also supported by government programs like Medicare and Medicaid, which began to recognize its potential in reducing healthcare disparities and improving access to care.
While these early uses were promising, it was not until the COVID-19 pandemic that telemedicine truly surged in popularity across the entire healthcare system.
COVID-19 and the Explosion of Telemedicine
When the COVID-19 pandemic struck in early 2020, it created a health crisis unlike anything the U.S. had ever seen. Hospitals were overwhelmed, and healthcare providers were faced with the dilemma of how to continue providing care while minimizing in-person interactions to reduce the spread of the virus. Telemedicine quickly became the answer.
Changes in Regulations and Reimbursement
In response to the pandemic, the U.S. government made rapid regulatory changes to support the widespread use of telemedicine. The Centers for Medicare and Medicaid Services (CMS) expanded telemedicine coverage under Medicare, including services that were previously restricted to in-person visits. This expansion included a broad range of services, such as primary care visits, specialist consultations, mental health therapy, and even some types of diagnostic tests.
The Federal Communications Commission (FCC) also introduced funding programs to support telemedicine infrastructure, including grants to help healthcare providers expand their capabilities for remote consultations.
On the private side, insurance companies were also forced to adjust. Many health insurers, including major companies like Aetna, Cigna, and UnitedHealthcare, relaxed their policies to allow for telemedicine reimbursement at the same rate as in-person visits. This shift made telemedicine a financially viable option for both providers and patients, increasing its adoption across the country.
Expansion of Telemedicine Services
As telemedicine became a viable option, healthcare providers across the country began to offer remote consultations for a wide variety of services. Virtual doctor visits became a routine part of healthcare for millions of Americans. Patients could consult with their doctors for common ailments like colds, flu, allergies, and more without leaving their homes. Many healthcare systems began to use telemedicine for follow-up care, mental health therapy, and even chronic disease management, especially for conditions like diabetes, hypertension, and asthma.
The convenience of telemedicine also helped reduce the strain on physical healthcare facilities. During the height of the pandemic, many routine procedures and non-urgent medical appointments were postponed, and telemedicine became a lifeline for maintaining healthcare continuity. Virtual visits allowed healthcare providers to monitor patients remotely, provide ongoing treatment, and keep track of patient progress, all while maintaining social distancing protocols.
Mental Health and Telemedicine
One of the most significant areas where telemedicine showed its potential was in the realm of mental health. With social isolation, fear, and uncertainty brought on by the pandemic, many Americans faced heightened levels of stress, anxiety, depression, and other mental health challenges. Telemedicine enabled individuals to access therapy and counseling from the comfort of their homes, which was particularly important for those in remote or underserved areas.
Telehealth platforms like Talkspace and BetterHelp gained enormous traction during the pandemic, providing online therapy through messaging, video calls, and phone consultations. Traditional mental health providers also adapted, offering virtual counseling sessions to patients, which helped address the surge in demand for mental health services during the crisis.
Telemedicine in the Post-Pandemic Era: The Future of Healthcare
As the pandemic eased in 2021, it became clear that telemedicine was not just a temporary solution but had become an integral part of the healthcare system. Patients and providers alike realized the benefits of telemedicine, which led to increased demand for its continued use. But what does the future of telemedicine in the U.S. look like in 2026 and beyond?
Telemedicine Expands Beyond Primary Care
While telemedicine’s initial rise was largely driven by primary care visits, it has now expanded to include specialized care, including services like cardiology, dermatology, and orthopedics. Remote consultations for managing chronic conditions, such as diabetes, hypertension, and asthma, have become common. Wearable devices and mobile apps that monitor health metrics like blood pressure, glucose levels, and oxygen saturation make it easier for healthcare providers to track patients’ health in real-time, improving outcomes and reducing the need for in-person visits.
For instance, telemedicine consultations can now be combined with home diagnostic tools like EKG monitors or pulse oximeters to gather real-time data, allowing doctors to diagnose and treat conditions remotely. The integration of telemedicine with these devices enhances patient care and reduces the need for patients to travel long distances to see specialists.
Increased Integration with Electronic Health Records (EHR)
As telemedicine continues to grow, its integration with Electronic Health Records (EHR) will become more seamless. EHRs are digital versions of patients’ paper charts and contain important health information like medical history, diagnoses, medications, and treatment plans. The integration of telemedicine with EHRs will enable healthcare providers to have immediate access to comprehensive patient data during virtual consultations, ensuring more accurate diagnoses and treatment recommendations.
This will also improve care coordination, as providers across different specialties and locations can easily share patient data, reducing the chances of errors and redundant tests. With the growing number of telemedicine platforms available, it is expected that interoperability with EHR systems will become more common, creating a more unified healthcare ecosystem.
Telemedicine in Rural and Underserved Areas
One of the most significant benefits of telemedicine is its ability to provide healthcare to individuals in rural and underserved areas. Access to healthcare has long been a challenge for people living in remote locations, where there may not be enough healthcare facilities or specialists to meet their needs. Telemedicine bridges this gap by enabling patients to consult with doctors from anywhere with an internet connection.
As broadband internet access improves and more telemedicine platforms are developed, the gap in healthcare access for rural and underserved populations will continue to narrow. According to the Federal Communications Commission, over 21 million Americans still lack access to reliable broadband, which is a significant barrier to telemedicine’s growth. However, efforts are underway to expand broadband infrastructure, especially in rural areas, which will further enhance telemedicine’s effectiveness.
Telemedicine and Remote Patient Monitoring
Remote patient monitoring (RPM) is one of the key advancements in telemedicine that is expected to grow significantly in the coming years. RPM allows healthcare providers to monitor patients’ vital signs and other health metrics in real-time, using wearable devices and mobile health apps. This is particularly useful for patients with chronic conditions like diabetes, heart disease, and respiratory illnesses, who require regular monitoring and care.
By combining telemedicine with RPM, healthcare providers can proactively identify potential issues and intervene before they become serious problems. This can help reduce hospital admissions, lower healthcare costs, and improve patient outcomes.
Challenges and Barriers to Telemedicine Adoption
While telemedicine has made significant strides in recent years, there are still several challenges that need to be addressed to ensure its widespread adoption and effectiveness.
Regulatory and Licensing Issues
One of the most significant barriers to telemedicine is the complex web of regulations and licensing requirements that vary by state. For instance, doctors are typically required to be licensed in the state where the patient is located, which can create issues when treating patients across state lines. Although there have been temporary allowances for cross-state telemedicine during the pandemic, permanent solutions to these regulatory hurdles will be necessary for the continued growth of telemedicine.
Technology and Internet Access
Access to the necessary technology and internet infrastructure remains a challenge, particularly for low-income and rural populations. While many people have smartphones and computers, not everyone has access to high-speed internet, which is crucial for high-quality video consultations. The U.S. government and private companies are working to address this issue by expanding broadband infrastructure, but there is still a long way to go.
Data Security and Privacy Concerns
As with any healthcare technology, telemedicine raises concerns about data